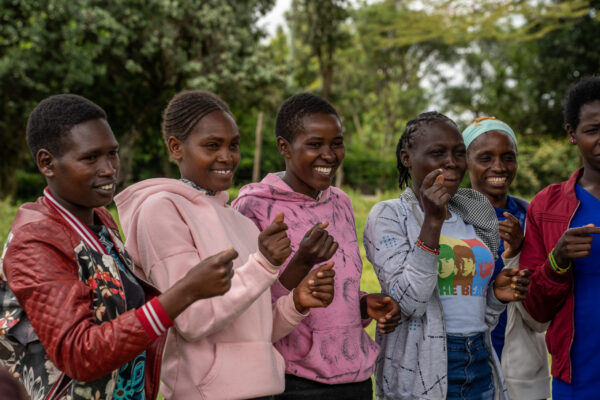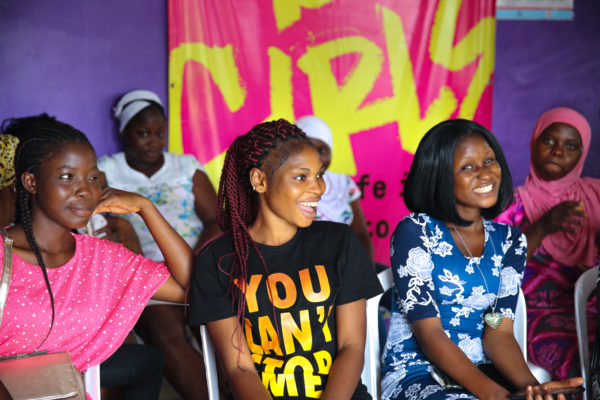By Christine Massawe, A360 Young Designer/Youth Officer, PSI Tanzania
Access to contraception is one of many tools that equips young people like me with the power to make the decisions that define our lives – even during COVID-19.
But with limited resources due to the pandemic, we’re seeing the divide widen between young people and our ability to make our reproductive health choices. In fact, according to research from the Guttmacher Institute, disruptions in sexual and reproductive health (SRH) programs as a result of the current pandemic could lead to 15 million unplanned pregnancies and 3.3 million unsafe abortions across 132 low- and middle-income countries over a 12-month period.
Prioritizing SRH access is a must, and our focus must remain on reaching young people who need SRH services, now more than ever. To serve young people, we need to understand young people – our specific needs and our unique experiences around life in pandemic. Our voices, by extension, must #BeThere, in the room where the programmatic and policy-based decisions happen around the solutions that serve us.
On Aug. 12, I joined young leaders from around the world on Twitter for #BeThere, a global chat that brought young people and “adults” together to not only hear but learn from young people as we discussed youth contraceptive access during COVID-19.
With voices from young leaders from my home country of Tanzania to those weighing in all the way from India, the conversation produced rich insights ripe with opportunity. We captured a summary, below.
We asked: How has COVID-19 changed how you make your health and life choices?
As youth participants shared: making decisions during COVID-19 is hard.
When it comes to finding SRH information during the pandemic, young people posted that they increasingly turn to online sources, including social media pages dedicated to health topics.
Still, while young people favor Facebook and WhatsApp, not all youth have access to data nor mobiles to log onto digital channels, many noted. And even when they do, not all SRH information that young people come across online is applicable to young people’s local context or presented in a digestible manner for young people to understand and/or connect to. It sounds simple but even the type of clothing depicted in accompanying photos matters – young people want to be able to see themselves. We shouldn’t target Nigerian youth with photos of young women in Indian saris.
The takeaway? To best reach and resonate with young people with access to digital sources, imagery, look and feel, presentation of information and language (including slang) should align with what young people know and trust based on their respective contexts.
As I’ve heard girls share in my own work supporting the design and delivery of PSI’s flagship youth contraceptive program Adolescents 360 (A360), young people face numerous challenges that can deter them from going to a clinic for SRH services. From judgmental providers who perpetuate the stigma around contraception to inconvenient hours that don’t work with our school or work schedules, young people like myself often find ourselves navigating one too many barriers when it comes to turning up for in-person support.
COVID-19 only heightens those obstacles.
Increased fear about contracting the virus from going to a clinic certainly stops many of us from showing up. But as young people shared during the Twitter chat, for those who do choose to go to the clinic for SRH services now, privacy and confidentiality still remain a point of concern.
How to solve? Young people shared ideas:
We asked: what are some of the main areas that ASRH programs overlook? What are some opportunities for growth?
As an A360 young designer, I’ve seen firsthand the value of co-designing ASRH solutions with and for the young people we serve. When it comes to delivering youth contraceptive programs that respond to youth needs – youth voices are still too often missed, young people said.
As a result, programs often miss accounting for young people’s holistic needs – including addressing menstrual health and hygiene (MHH), a component that young people stressed as “imperative” to delivering a comprehensive package of youth SRH services. After all, misperceptions behind bleeding changes as a result of contraceptive use remain common. Countering these myths by including MHH programming could support girls to feel comfortable to choose and stay on a contraceptive method that works best for them – now, and beyond COVID-19.
We can innovate in how we reach young people, on their own terms. Self-care interventions, specifically, offer people everywhere – and young people, especially – the ability to take charge of our own health, leading to improved outcomes in areas in which stigma may prevent us from seeking care. I’m excited to see where we go next.
We asked: what makes you feel supported to meaningfully contribute your voice and expertise to designing youth SRH programs?
Simple: start by listening to and trusting young people.
“Adults” have the opportunity to bring us young people into the story as we, together, drive toward a reality in which every young person can use our voices to choose our futures.
After all, young people’s lives – our dreams, our choices – don’t pause for pandemics.