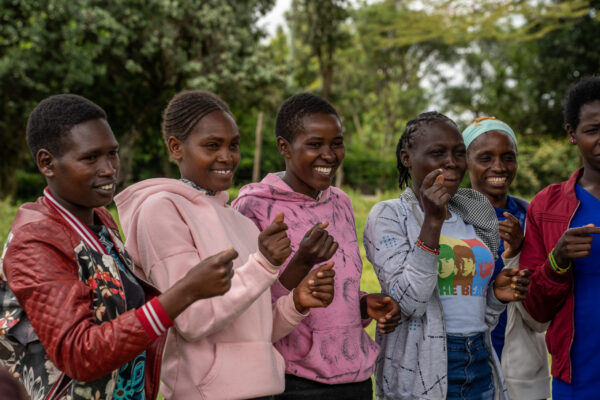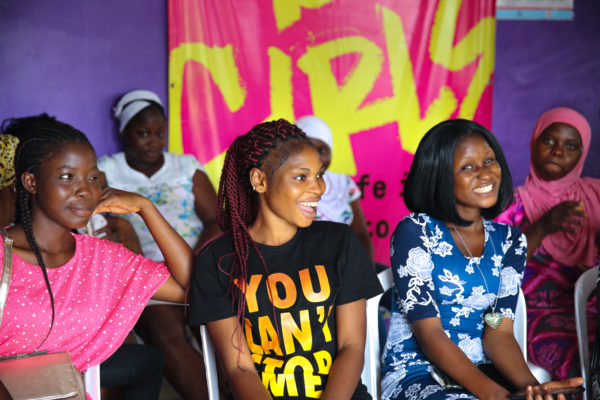This is part one of our series on A360 Ethiopia’s experience designing and testing Smart Start’s adaptation for in-school girls. Read part two for the team’s takeaways from testing their prototype remotely.
By Ruth Desta, Sexual and Reproductive Health Program Manager, PSI Ethiopia
As our program insights show: in Ethiopia, unmarried girls in relationships may not plan to have sex – as they shared, “it just happens!”
And still, stigma and misperceptions continue to stand between unmarried girls and their ability to choose contraception.
Through A360, we’ve learned that when we bring young people in as co-designers of the solutions that serve them, we, together, can deliver programs that support girls to see the relevance of contraception to their lives.
It’s a model ripe for replication – and one we, the A360 Ethiopia team, used as we expanded our focus to respond to the needs of unmarried Ethiopian girls too often left behind.
Started with Married. Expanded to Unmarried.
A360 sought to change that. We – PSI/Ethiopia in partnership with young people and the Federal Ministry of Health (FMOH) – developed Smart Start, a girl-centered contraceptive program that supports rural, married girls aged 15-19 and their husbands to understand the cost-benefits of delaying pregnancy. We responded to young couples’ desires to achieve better futures and introduced contraception as a tool in support of those goals.
While Smart Start was developed for rural, married girls, we knew that the A360 approach delivered a strong foundation to reach and serve unmarried, urban girls aged 15-19.
With funding from Maverick Collective, PSI’s philanthropic initiative, we, alongside young people, sought to serve in-school girls in Mekele, Tigray region.
Which is when young people reinforced that yes, even amidst stigma around sex before marriage, unmarried girls in relationships are having sex.
In Ethiopia, four in five girls will have their first baby by age 20, often before they understand the financial implications of having children before they are ready. Many of these pregnancies are unintended. Reaching this cohort with ASRH information and services remains paramount.

What Girls Told Us
Away from home, exposed to new cities, ideas, and–of course–boys, girls face higher risks for unwanted pregnancy.
Yet, young people shared, girls often feel uncomfortable approaching health providers for ASRH information and services for fear of judgement or, worse yet, being turned away.
Our A360 team tested prototypes of school-based contraceptive counseling programs and found that both girls and boys feel that school is a safe place for them to receive SRH information and services, because they want services that are private and confidential.
However, school-based, Western-funded SRH projects face resistance from communities. Many fear that global NGOs and donors will infuse SRH education with Western culture and, by extension, encourage adolescents to have sex from an early age.
Moreover, our insight gathering phase showed that while education administrators want students to engage in sexual education, they’re cautious about what and how much information reaches students for fear it may encourage young people to have sex.
And while our program didn’t have the time nor resources to respond to this specific challenge, we did take extra steps to ensure transparency in our communication with school administrators. The MoU that was signed between health, education regional bureaus and PSI gave us legal framework to implement the program.
Through multiple iterations – and some adaptations to account for COVID-19—we landed on a solution: programming that starts the conversation with girls’ dreams, with contraceptive services provided, on-site, on-demand and for free.
Before COVID-19
Before COVID-19, girls received contraceptive counseling in schools. The Ethiopian government’s policy, however, doesn’t allow for service delivery in secondary schools As a result, girls dropped off – opting out of seeking service delivery after their school-based counseling session.
In contrast, in technical and vocational education and training (TVET) schools, government policy permits contraceptive service provision as TVETs are considered college level institutions. In fact, in our preliminary research, of the 6 girls counseled and offered on the spot service, 4 voluntarily took method.
Our takeaway? Counseling should be followed by immediate service provision. As a result, counseling should be provided in a place where the service, itself, happens.
Adapting for COVID-19
During COVID 19 where girls are no longer in school, we took the counseling to girls’ homes. Similarly, no girl opted in for services after counseling. But when we reached girls away from home with on-site service delivery, and in an environment in which they told us they felt comfortable in, they chose contraception. In our early research, we counseled 5 girls away from home. 4 chose a method.
Later, when we partnered with the Family Guidance Association Ethiopia (FGAE), we offered on-site delivery at youth health clinics in FGAE’s youth centers. There, 288 girls (145 secondary and 143 TVET) were counseled through trained counsellors, and 48 girls (20 secondary and 28 TVET) voluntarily adopted both short and long acting methods.