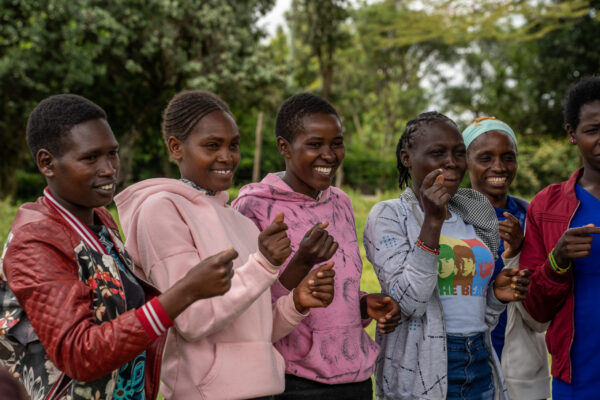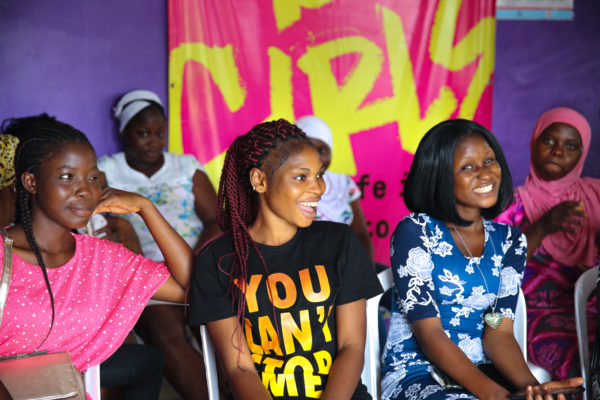This piece is a part of A360’s replication series on the UK Aid-funded Vale-a-Pena project. With and for young people, Vale-a-Pena is proving the power in applying A360’s youth-powered approach to determine what it takes to enact effective, resonant and ultimately lasting adolescent and youth sexual and reproductive health (AYSRH) behavior change in Mozambique – and beyond.
By Fuva Muiambo, Communications Officer, PSI/Mozambique
Erdinha Chambal, a nurse in the Mozambican district of Mandjacaze, knows what women in her community want when it comes to contraception. For her, the most popular methods she provides have always been short-term options.
“Most of women that came into the health facility leave with a pica (a local word for a contraceptive injection) or oral contraception,” explains Erdinha. “They are afraid that the implant will disappear into their bodies or make them infertile.”
In Mozambique, research from the Ministry of Health has shown that despite the availability of long-acting reversible contraceptives (LARCs), like implants and IUDs, only 6.46% of women who use contraception choose a long-acting method. Many providers don’t know how to counsel their clients about long-term methods or how to provide them. Their clients don’t ask for them, either, resulting in very little demand for LARCs.
Informed choice—when a client can choose the best contraceptive for her needs based on a thorough understanding of the methods available to her—is an important part of avoiding unintended pregnancy. A girl’s informed decision depends on a comprehensive sexual and reproductive health session with a skilled and motivated health provider, who must feel comfortable in explaining and administering all available methods.
In response to this lack of informed choice, PSI Mozambique has been implementing activities in the districts of Chibuto and Mandjacaze that complement the youth-focused interventions being implemented by the UK Aid-funded Vale-a-Pena project. These activities provide on-the-job training to health providers on the fully array of available contraceptive options, which in turn creates demand for voluntary contraceptive services and improved delivery of these services. So far, PSI Mozambique has completed a total of 27 three-day outreach campaigns for health providers.

When PSI’s team came in to offer the training at Erdinha’s health facility, she was thrilled.
“It was something new for us, we don’t usually have trainings in the health facility,” Erdinha said.
The support that PSI Mozambique provided allowed Erdinha and her team to learn new ways of counselling, placing a focus on the importance of informed choice, including the benefits and side effects of all available contraceptive methods.
“Since the most popular methods were oral contraceptives and injectables, we wouldn’t talk [to clients] about implants or IUDs,” Erdinha recalls.
The counselling tools Erdinha was taught helped demystify common myths around the various available contraceptive methods. She said that it was also helpful that a specialized nurse was available to train them on-the-job on how to administer long-term methods.
“With the PSI team, we were able to review LARC administration techniques. It was a great refresher, since we weren’t used to doing it before,” Erdinha asserted.
With improved contraceptive counselling and technical skills, Erdinha felt much more confident talking to adolescents about all the methods of contraception available to them.
“When Maria, a 16-year-old girl came to the health unit asking for health counseling on contraception, I was able to have a friendly conversation with her and explained all the options she has,” Erdinha remembers with pride. “She spoke about her future and her interest in finishing her studies, and chose an implant.”

Learn more about how Mozambique’s Vale-a-Pena intervention is applying the A360 Blueprint for AYSRH Change to reimagine how young Mozambicans access modern contraception, today.